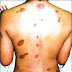
Toxoplasmosis (toxo) is an infection caused by a single-celled parasite called Toxoplasma gondii .The infection is most commonly acquired from contact with cats and their feces or with raw or undercooked meat.
Toxoplasmosis (toxo) is an infection caused by a single-celled parasite called Toxoplasma gondii .The infection is most commonly acquired from contact with cats and their feces or with raw or undercooked meat.The U.S. Centers for Disease Control and Prevention (CDC) estimates that more than 60 million people in the United States may carry the Toxoplasma parasite, but very few have symptoms because a healthy immune system usually keeps the parasite from causing illness.
 What factors increase the risk of acquiring toxo?
What factors increase the risk of acquiring toxo?The following situations potentially expose a person to the toxoplasma parasite and increase the risk of acquiring toxoplasmosis:
touching your hands to your mouth after gardening, cleaning a cat's litter box, or anything that came into contact with cat feces
eating raw or partly cooked meat, especially pork, lamb, or venison
touching your hands to your mouth after contact with raw or undercooked meat
organ transplantation or transfusion (this is rare)
If a woman is pregnant when she is infected with toxo, the infection can be transmitted from her to the baby with sometimes catastrophic consequences.
What are the usual symptoms of toxoplasmosis?
Although people infected with toxoplasmosis are often unaware of having this disease, typical symptoms of toxo are flue like symptoms including swollen lymph nodes and muscle aches and pains that last from a few days to several weeks. If your immune system is normal, you cannot get the infection again.
Why do some people develop severe problems from toxo?
Few people with toxo develop symptoms because the immune system usually keeps the parasite from causing illness. However, anyone with a compromised immune system is at risk for serious problems from toxo. These individuals include those undergoing chemotherapy, people with HIV/AIDS or other immune disorders, and recent organ-transplant recipients.
In these people, an infection that occurred anytime during life can reactivate and cause the severe symptoms of toxoplasmosis such as damage to the eye, brain, or other organs.
Ocular toxoplasmosis, which damages the eyes, can lead to reduced vision, blurred vision, pain (often with bright light), redness of the eye, and sometimes tearing, according to the CDC.
Can toxoplasmosis develop into a more serious illness in babies?
Yes, the immune system in infants is not fully mature until after birth.
The babies of women who were exposed to toxo within a few months of becoming pregnant or during pregnancy are at an increased risk for developing a severe case of toxo. According to the NIH (U.S. National Institutes of Health), pregnant women who newly contract the toxoplasmosis parasite have a 40% chance of transmitting it to their unborn child. Women who were first exposed to toxo more than six months before becoming pregnant are not likely to pass the infection to their children.
Most infants have no symptoms at birth, but a small percentage may be born with eye or brain damage. Unfortunately, the signs and symptoms of the disease often appear a few months after birth.

What is meant by a baby developing "a more severe case of toxo"?
Children born with toxoplasmosis can be afflicted with mental retardation, convulsions, spasticity, cerebral palsy, deafness, and severely impaired vision. The infant's head may be abnormally small (microcephaly) or abnormally large due to increased pressure on the brain (hydrocephalus).
How is toxo diagnosed in the lab?
There are many different kinds of blood tests for toxoplasmosis. The results can determine if the patient has had toxo and whether the infection is recent ("acute") or not.
How can toxoplasmosis be prevented?
Since toxo usually causes mild to no symptoms, and a healthy immune system prevents any remaining parasites in the body from causing further symptoms, most people don't need to worry about getting this disease.
However, if you have a weakened immune system or are pregnant, there are several steps you should take to prevent exposure to toxoplasmosis.
If you have a weakened immune system, get a blood test for toxoplasmosis. If your test is positive, your doctor can tell you if and when you need to take medicine to prevent the infection from reactivating.
If you are planning on becoming pregnant, you may consider being tested for toxo. If the test is positive, there is no need to worry about passing the infection to your baby (since you should have immunity against the parasite).
If you are already pregnant, you should discuss your risk of toxoplasmosis with your doctor who may order a blood sample for testing.
Wear gloves when you garden or do anything outdoors that involves handling soil since cats often use gardens and sandboxes as litter boxes. Wash your hands well with soap and warm water after outdoor activities, especially before you eat or prepare food.
Have someone else handle raw meat for you. If this is not possible, wear clean latex gloves and thoroughly wash with soap and hot water any cutting boards, sinks, knives, and other utensils that might have touched the raw meat. Wash your hands well with soap and warm water afterward.
Cook all meat thoroughly, especially pork or veal.

Yes, but if you have a weakened immune system or are pregnant, there are some steps to take to avoid being exposed to toxo according to the Cornell College of Veterinary Medicine.
Most importantly, you can help prevent your cats from getting infected with toxo. Feed them dry or canned cat food and keep them indoors. Cats can become infected by eating or being fed raw or undercooked meat that is infected with the parasite, or by eating infected prey such as birds or rodents. Any cat that is allowed access to outdoors should be kept off beds, pillows, or other furniture that you also use. Don't bring a new cat into your house that might have been an outdoor cat or might have been fed raw meat. Avoid handling stray cats and kittens. Have your cat tested for the parasite. Your vet can answer any other questions you may have regarding your cat and the risk for toxoplasmosis.
Have someone who is healthy and not pregnant change your cat's litter box. If this is not possible, wear gloves and clean the litter box daily (the parasite found in cat feces needs a few days after being passed to become infectious). Wash your hands well with soap and warm water afterward.
Once infected with toxo, is my cat always able to spread the infection to me?
No, cats can only spread toxo in their feces for a few weeks after they are first infected with the parasite. Like humans, cats rarely have symptoms when first infected, so most people don't know if their cat has been exposed to toxo. In fact, most infected cats appear healthy. There are no good tests available to determine if your cat is passing toxo in its feces.
What is the treatment for toxoplasmosis?
Once the diagnosis of toxoplasmosis is confirmed, you and your doctor should discuss whether treatment is necessary. In an otherwise healthy person who is not pregnant, treatment is not needed. Symptoms will usually go away within a few weeks. For pregnant women or people who have weakened immune systems, drugs are available to treat the parasite that causes toxoplasmosis.
Toxoplasmosis At A Glance
· Toxoplasmosis (toxo) is a disease caused by a parasite.
· Toxo is acquired from contact with cats and their feces.
· Toxo is also acquired from eating or touching raw or partly cooked meat.
· Symptoms can range from none to very severe.
· A woman who contracts toxo right before or during pregnancy can transmit it to her baby with catastrophic consequences.
· People with immune deficiencies are at high risk for developing severe signs and symptoms of toxo.
Featured:
Toxoplasmosis (toxo) is a parasitic infection that causes flulike symptoms, swollen lymph nodes, and muscle aches and pains that may last from a few days to several weeks. Pregnant women who contract toxo have a 40% chance of passing the infection to their babies. Babies born with toxo may be afflicted with mental retardation, cerebral palsy, deafness, and severely impaired vision.
Medication for Toxoplasmosis
GENERIC NAME: PYRIMETHAMINE - ORAL (pir-ih-METH-uh-meen)
BRAND NAME(S): Daraprim
USES: This medication is used in the treatment and prevention of prevention of malaria or the treatment of Toxoplasmosis (a parasitic infection). Pyrimethamine is often taken in combination with other antimalaria medication.
HOW TO USE: Take this medication by mouth with food or meals as directed. For preventing malaria, this is usually taken once a week. For treatment of a malarial attack, this is taken once a day for 2 days, then given once a week. In the treatment of toxoplasmosis, this may be given once or twice a day for up to 5 weeks. Take this medication for the full time prescribed. Stopping therapy too soon may result in ineffective treatment.
SIDE EFFECTS: Nausea, stomach upset or loss of appetite may occur especially the first several days as your body adjusts to the medication. Other effects reported include headache, lightheadedness, dry mouth, diarrhea, trouble sleeping. If any of these effects continue or become bothersome, inform your doctor. Notify your doctor if you develop a sore throat, unusual bruising, pale skin, swelling of the tongue, depression, irregular heartbeat. Use caution driving or operating machinery if this medication makes you lightheaded. This medication may cause blood disorders. It is important that lab tests be done periodically while taking this medication to monitor for this. A serious allergic reaction to this drug is unlikely, but seek immediate medical attention if it occurs. Symptoms of a serious allergic reaction include: rash, itching, swelling, dizziness, trouble breathing. If you notice other effects not listed above, contact your doctor or pharmacist.

A is for animals, Z is for zoonoses.
They come from giant Gambian rats and fuzzy bunnies. They come from puppies and pythons. Whether the animal is friend or food or foe, it can carry dangerous diseases.
There are at least 39 important diseases people catch directly from animals. There are at least 48 important diseases people get from the bite of bugs that bit an infected animal. And there are at least 42 important diseases that people get by ingesting or handling food or water contaminated with animal feces.
Some are as old as memory: rabies, bubonic plague, food poisoning. Others have only recently emerged: monkeypox, West Nile encephalitis, Legionnaires' disease. And some, such as highly lethal bird flu, we fear even though they haven't -- yet -- spread in humans.
People have lived with animals for eons. There's a reason for that. They don't just make us feel better. They actually contribute to our health. People who keep pets tend to have lower cholesterol levels and lower blood pressure. They tend to get more exercise and to feel less lonely.
On the other hand, pets and other animals can get sick. And some of these illnesses can be quite dangerous. This article offers an overview of these diseases -- and how to avoid them.
Why Animal-Borne Diseases Matter
Diseases passed to humans from animals are called zoonoses. What makes one of these diseases important? Two things, "If you ask Americans in general what is the most important zoonosis, most would say rabies," "It is something they fear, it is in the news. But in terms of risk, there are only zero to two human cases a year in the U.S. It's one of those zoonoses that are important because of their seriousness, but not their frequency: rabies, tularemia, plague, monkeypox, listeria, anthrax. These are diseases that are very serious if one gets them but which are relatively uncommon."
On the flip side, are animal-borne diseases that are important because they are fairly common even if not often fatal. Cat-scratch fever, for example, infects as many as 20,000 Americans a year. And an estimated 4%-20% of U.S. kids get roundworm from dogs and cats.
 Toxoplasmosis
ToxoplasmosisCats allowed to roam outdoors often pick up a parasite known as Toxoplasma gondii. Most of the time, the cat will fight off the infection before it becomes contagious. However, sometimes cats shed egg-like forms of the parasite in their feces. That's why pregnant women, small children, people with damaged immune systems, and people on cancer chemotherapy should avoid cleaning cat litter boxes.
Usually, a person who gets toxoplasmosis gets very few symptoms. But when a person does get the disease, it causes a flu-like illness and/or muscle aches and pains lasting for a month or even longer. "A very sizeable proportion of humans -- 30%-40% -- have been infected with toxoplasmosis, usually by eating undercooked meat," Glickman says. "Most people never had a symptom or had very mild disease. But in people [with weakened immune systems] it can be fatal. And the worst infections may be in pregnant women. The organism can go to the fetus and, if the baby doesn't die, cause lifetime illness."
Diseases from Cats and Dogs
By far they're our best friends. And that means cats and dogs are common sources of disease.
Cats often carry a germ called Bartonella henselae. Some 40% of cats are infected at least once in their lives -- usually when they're kittens -- but they don't look sick. Humans get infected only when they are bitten or scratched by an infected animal -- cat-scratch fever

Other bacterial infections humans can get from cats and dogs include:
Plague. Rodents carry the plague bacteria. Very rarely, cats get fleas from infected rodents and pass the disease to humans.
Q fever.
People are much more likely to get Q fever from barnyard animals than from cats. But it does happen. Half of infected people get symptoms that include fever, headache, chest or stomach pain, diarrhea, and/or vomiting. It can also cause temporary swelling of the heart -- a dangerous event for people who already have heart disease.
Campylobacter infection. Found in animal feces, this germ causes gastrointestinal symptoms. It's usually not dangerous, but can cause severe illness in people with weakened immune systems.
Leptospira infection.
Humans get infected via contact with water, food, or soil containing urine from infected animals. Left untreated, leptospirosis can be quite serious. It can lead to liver failure, trouble breathing, kidney damage, brain and spinal cord infection, and, rarely, death. Symptoms vary widely but can include high fever, severe headache, chills, muscle aches, and vomiting. There may also be yellow skin and eyes, red eyes, abdominal pain, diarrhea, or a rash.
Salmonella
infection. People get this often-severe gastrointestinal infection via contact with animal feces. It can cause severe kidney damage to young children.
Both cats and dogs sometimes get parasites that infect humans. One of the most common is roundworm. Left untreated, nearly all puppies and kittens pick up this parasite. Its egg-like form -- the oocyst -- can survive for years in soil.
When humans ingest oocysts, tiny worms hatch in the gut and move through the body. Symptoms include fever, coughing, asthma, and/or pneumonia. Once in a while, the tiny worms enter the eye and scar the retina. This results in permanent partial vision loss. "Some 750 to 1,500 kids go blind each year with roundworm infection [of the eyes] passed from dogs through feces to children.
Other parasites of cats and dogs:
 Tapeworm.
Tapeworm. A person gets infected by swallowing an infected flea -- a relatively rare event, but it happens.
Hookworm. Hookworms are common in tropical and subtropical areas. They infest soil contaminated by animal feces. Humans get infected by direct contact, usually by walking on contaminated soil. Heavy infections can be serious.
Cryptosporidiosis.
This parasite cause mild to severe intestinal symptoms like diarrhea. It's not usually a dangerous infection, except to people with weakened immune systems.
Ringworm
isn't a parasite, but a fungal infection that forms a ring-shaped rash on the skin or a bald patch on the scalp. People can get it from direct contact with an infected animal.
Cats and dogs get viruses, too. Rabies is the most dangerous one. Be sure to keep up with your pet's rabies vaccination.
To protect yourself from diseases carried by house pets:
· Wash your hands with soap and running water after touching feces.
· Take your pet to the vet on a regular basis and keep up with all vaccinations recommended for your area.
· Avoid rough play with cats.
· If your cat or dog bites you, wash the area with soap and water right away.
· Wash your hands after handling your pet -- especially before eating or preparing food.
· People with weakened immune systems should take special precautions. These include never letting pets lick them on the face or on an open cut or wound, never touching animal feces, and never handling an animal that has diarrhea.
· Don't let your pet drink from toilet bowls or eat feces.
 Other Pets, Other Diseases
Other Pets, Other DiseasesWe humans have other friends besides cats and dogs. And with these other friends come other diseases:
Birds. Pet birds, including parrots and parakeets, can spread psittacosis. It's a relatively rare disease, with about 50 U.S. cases each year. Symptoms include fever, chills, headache, muscle aches, and a dry cough. There's often pneumonia, which can be quite serious and even fatal. Untreated infections can lead to serious heart, liver, and nerve problems.
Reptiles and amphibians. Snakes, turtles, lizards, frogs, toads, and salamanders -- like other animals -- can carry Salmonella bacteria. Wash your hands after handling them. Keep them in their habitat; don't let them wander your room. Keep reptiles and their equipment away from the kitchen. Don't clean reptile cages in sinks or tubs used by people. Don't kiss your reptile -- it won't like it, anyway. And keep reptiles and amphibians away from children younger than 1 and people with weakened immune systems.
Exotic animals. Yes, some people make pets of animals like African pygmy hedgehogs. These tiny, antisocial animals that roll up into spiky balls were a fad not too long ago. And they came with salmonella. More recently, pet Gambian giant rats brought monkeypox into the U.S. Similar to smallpox -- but fortunately milder and not as contagious -- monkeypox lurks in small mammals in the African rainforest.
Wild Animals
Wild animals should stay that way. Enjoy them from a distance. Even so, they're a rich source of human disease. Here are a few:
Raccoon roundworm.
This is the best reason not to feed wild racc
 oons. The feces of an infected raccoon carry millions of roundworm eggs. These eggs become infectious in two to four weeks and can survive for years in the environment. They are very difficult to kill -- the CDC recommends cleaning contaminated decks or porches with boiling water or a propane flame gun (with proper caution, of course).
oons. The feces of an infected raccoon carry millions of roundworm eggs. These eggs become infectious in two to four weeks and can survive for years in the environment. They are very difficult to kill -- the CDC recommends cleaning contaminated decks or porches with boiling water or a propane flame gun (with proper caution, of course).Symptoms depend on where the roundworms travel in the body. They can include nausea, fatigue, enlarged liver, and symptoms of brain infection (poor coordination, inattention to one's surroundings, loss of muscle control, coma, and/or blindness). Some infections have been fatal. Diagnosis is difficult. If you are having symptoms after contact with raccoons, be sure to tell your doctor. There is no specific cure, but early treatment can limit the extent of disease.
Giardia infection. This microscopic parasite is the hiker's bane. It's one of the main reasons why you should always purify water taken from a stream, no matter how far from civilization you're camping. An infected animal sheds Giardia in its feces. It can survive for a long time in water and in soil.
 Symptoms include, loose or watery diarrhea, stomach cramps, and stomach upset. People with Giardia infection are contagious and easily spread the parasite to others. Fortunately, there are excellent curative treatments.
Symptoms include, loose or watery diarrhea, stomach cramps, and stomach upset. People with Giardia infection are contagious and easily spread the parasite to others. Fortunately, there are excellent curative treatments.Hantavirus.
Lymphocytic choriomeningitis (LCM).
This is a virus spread by the common house mouse. The virus can infect the linings of the brain and spinal cord. It's a serious disease, although many people get only mild infections. Mice shed the virus in their urine, saliva, and feces. People get infected by eating contaminated food or by inhaling aerosolized mouse urine or feces. LCM has two phases. The first lasts about a week and begins with fever, loss of appetite, head and muscle aches, nausea, and/or vomiting. There may be other symptoms as well. The second phase happens just as the first one gets better. It may begin with symptoms of meningitis: fever, headache, and stiff neck. It may also begin with symptoms of encephalitis: sleepiness, confusion, and movement problems. There's no cure, but most people recover completely with supportive treatment. However, some people are left with permanent nerve or brain damage. About 1% of people with LCM die.
 Tularemia (rabbit fever).
Tularemia (rabbit fever). People usually get tularemia from direct contact with rabbits. A person can also get it via the bite of an infected tick or deerfly, by eating contaminated food, by drinking contaminated water, or by breathing in F. tularensis, the bacteria that causes rabbit fever. It's very infectious: Fewer than 10 microscopic germs can cause a lethal infection. This is why tularemia was studied during World War II as a germ warfare agent. The kind of disease one gets depends on how one is infected. The inhaled form is most severe, with a 30%-60% fatality rate in untreated cases. It causes pneumonia with sudden fever, chills, muscle and joint aches, dry cough, and progressive weakness. In severe cases there is bloody spit with difficulty breathing.
Equine Encephalitis and West Nile Viruses
The equine encephalitis and West Nile viruses are transmitted from wild birds to humans -- and to horses -- by mosquitoes. It can cause a very dangerous infection of the brain and spinal cord. So can equine encephalitis, which has long been firmly rooted in the U.S. In fact, eastern equine encephalitis is considered a much more serious disease. About 30% of people who get it die, and another 30% have lasting nerve damage.
Most years there are very few cases of equine encephalitis. But some years are much worse than others -- and there's no way to predict in advance when there will be an outbreak.
Ebola Virus
It's hard to think of a more horrible disease than Ebola hemorrhagic fever. Ebola virus is spread by contact with the blood or body fluids of an infected person. Does it come from animals? Probably. Monkeys and great apes get it -- and people can get it from them when they butcher them for food. But monkeys die of Ebola, so they can't be the ultimate host. Most researchers think there's an animal out there harboring the virus. They just haven't found it yet.
 SARS
SARSThat SARS emerged in China's Guangdong province seems sure. What's not sure is where it came from. SARS is a coronavirus, but it's not like any other member of the coronavirus family. Some researchers think it may have come from an endangered animal known as a masked palm civet -- like most exotic animals, a culinary delicacy in parts of China. Others find the evidence weak. Whether SARS evolved in animals or humans remains a matter of debate.
Influenza, bird flu viruses
One disease that's definitely evolving in animals is influenza. And one place it's evolving is none other than Guangdong, China, where animals are kept in close proximity to one another. Flu viruses tend to arise in ducks and geese. They spread to chickens and to pigs. Pigs can also get infected with human flu viruses, so they make a good mixing pot for new flu. When an animal or a person is infected with two different flu viruses, the viruses like to swap parts. Voilà! A new virus emerges.
Infectious disease specialists don't wonder whether there will be a new worldwide flu epidemic. They only wonder when it will happen. There have been two recent close calls.
In 1997, lethal bird flu arose in the poultry markets of Hong Kong. People got infected and died, but the slaughter of millions of chickens stopped the virus before it learned how to spread from person to person. In 2001 and 2002, similarly bird flu viruses evolved in Hong Kong chickens. Fortunately, they didn't spread to humans.
What Puts Us At Risk?Animals can pass parasites on to humans. Children should not kiss or be kissed or licked by pets. This is a very easy pathway for parasites to enter the human body. Keep infants and toddlers away from pets that have not been wormed.
Hands should be washed after each and every contact with a pet, otherwise one is putting self at serious risk.
Animals that are strictly indoor animals and that do not come into contact with the outdoors are a much lesser risk, but still a risk. Animals that come and go from the outdoors into the home pose a serious risk, especially to children. Cats and dogs for example clean their anus with their tongues. If they lick you, they are transferring parasites to your skin. If they lick your face, it does not take long for the parasite to find its way into your mouth and your intestine.
Toxoplasmosis and is usually acquired from cats. A small scratch from a cat or dog can also transmit the parasite. Cats use a cat box. They are moving around feces and urine that has been prior deposited in the cat box. This dirt that has parasites.
Cat boxes should be scooped daily and thoroughly bleached and washed on a weekly basis.
Make sure you use gloves; put two pair on when doing this. Use HOT water with the bleach. If you do this is in a bathtub, make sure you bleach and disinfect the bathtub afterwards to kill any bacteria or parasites. Its' best to clean the box outside. Mechanical cat boxes are a breeding ground for bacteria and parasites because you cannot easily disinfect them.
Dogs are no different because they also lick their anus. If you have a pet that is stretching its' behind on your carpet, you better get that pet to a vet to get wormed. You should also steam clean, at least three times a year, your carpet. Parasites can be transmitted to carpets from shoes and animals. Never walk barefoot on carpet, especially near doors. Cats should definitely be kept away from new born and infants less than three year olds. A parent that gets that sweet little kitty for their one year old is playing Russian roulette with their child's life. Parasites can exist on the fur as well. Indoor animals should be bathed regularly just like animals, twice a month, at least! And if it is an outdoor animal that comes indoors, do not let the animal lay on furniture, you are only inviting health problems.
You may think this is taking things to an extreme, but believe me, these deadly little parasites are on those dear loving pets of ours. If you own a cat, keep in strictly indoors, never let it go outdoors. If you practice these recommendations, you will find you will have less health problems. Do not under any circumstance; give your pet raw meat of any kind. You are providing the means for a parasite infection in the pet which can easily be transmitted to humans, especially children. Do not let your children play in areas where animals have defecated without spraying the area with bleach.
Animal feces should be picked up using a shovel daily and gloves should always be worn and hands washed thoroughly after any yard work. Wear a air filter mask while you do this if they area is dusty. The dust you breathe in will contain parasites. By the way, any garden work, always wear gloves. There are over 100 different parasites in soil that can be transmitted from the soil. Never work in soil if you have a cut on your hands. The little critters will get into your bloodstream via the cut. Do not flush cat box liter down the toilet. The parasites can cling to the bowl and crawl up to the seat. Once on the seat, they find their way into you. If you see rice like particles coming out in animal feces, they have worms or parasites.
Fleas are carriers of tapeworms. Recently a woman in New Jersey had severe lower colon pains and severe bloating. This went on for several months. She had two dogs in her house that she let outside every day. Several months after trying to cope with the colon pains, she then developed rashes and itching. Nine months later, they found through exploratory surgery, a large 3 and 1/2 foot tape worm inside her and several smaller ones. Upon investigation at her house, fleas were found in the carpet. Do not walk barefoot around animals unless they are strictly an indoor animal.